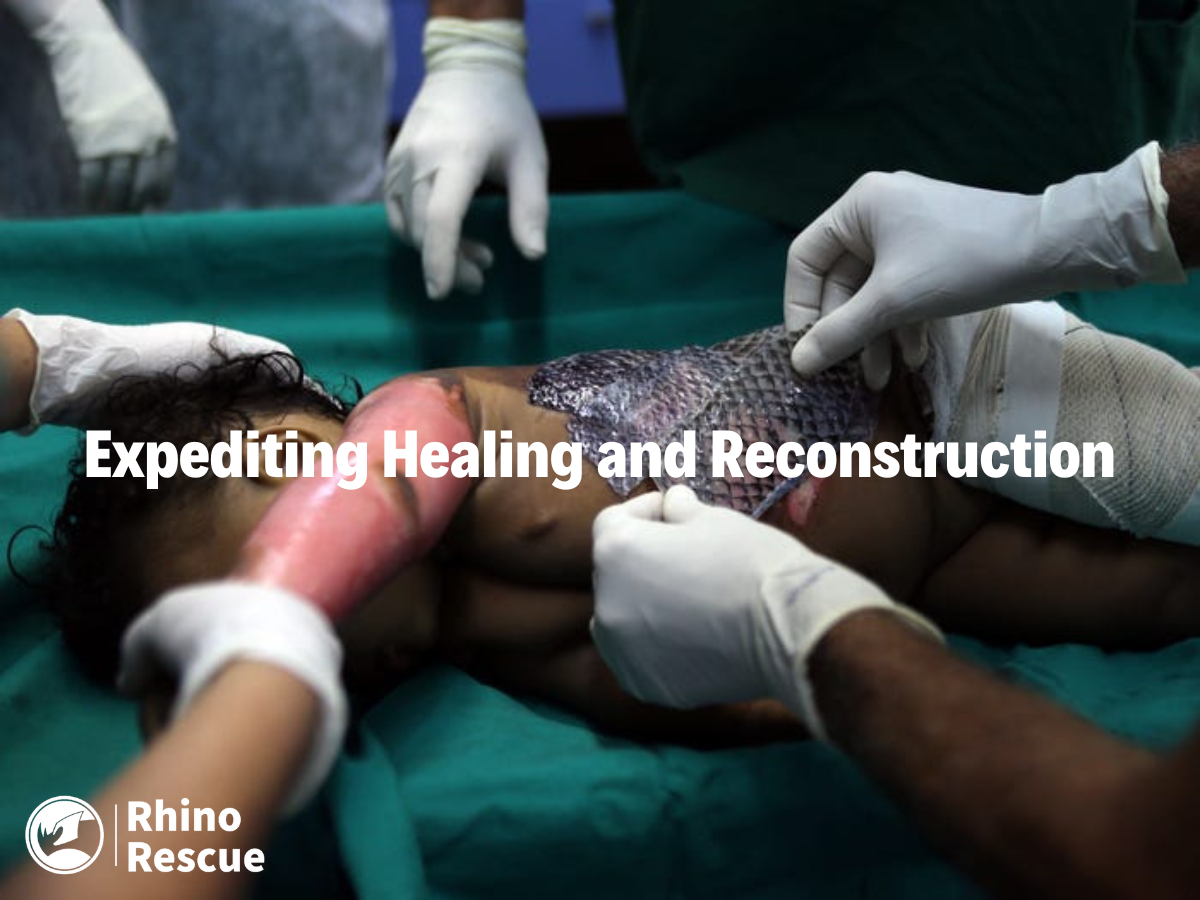
This blog article discusses the application of fish skin grafts for burn treatment under field conditions and in burn treatment. Fish skin grafts offer advantages such as infection prevention, pain relief, and faster wound healing. .

Fish skin grafts were used to treat severe burns and blast injuries. By facilitating granulation and revascularization, fish skin grafts expedited wound healing, allowing earlier grafting and reconstruction.
Advances in Burn Treatment and Medical Aid during the Nagorno-Karabakh War
The Nagorno-Karabakh War, a significant armed conflict between Azerbaijan and Armenia in 2020, centered around a region with deep ethnic and historical significance. Spanning from September 27 to November 10, the war witnessed a notable shift in warfare tactics, with the widespread use of drones for reconnaissance and targeted airstrikes. These technological advancements, along with the deployment of long-range weapons and sensors, marked the dawn of a new era in warfare.

Expanding and Restructuring
During this conflict, the use of drones introduced a new dimension of battlefield injuries. While the specific ammunition used in drone combat remains unclear, there have been reports of white phosphorus compounds being employed. Exposure to these substances can lead to severe chemical burns, resulting in high morbidity rates and prolonged hospital stays. Notably, these burns predominantly affected exposed areas of the skin, such as the face and hands, leading to an increase in flash burns compared to traditional combat scenarios. Additionally, explosions and gunshot wounds further contributed to the diverse range of injuries, including thermal and chemical burns.
The overwhelming number of casualties faced by both sides strained Armenia's military hospitals beyond their capacity. As a result, civilian hospitals were repurposed to treat wounded soldiers. Many injured personnel were transported directly from the battlefield to the capital's hospitals. Unfortunately, due to the overwhelming demand, timely surgical interventions were often delayed, with patients enduring waits of more than a week. In the interim, burn dressings were regularly administered, and high doses of opiates were utilized to manage excruciating pain. The burns observed in the conflict primarily consisted of deep partial-thickness or full-thickness burns.
To address the challenges posed by partially excised burn wounds, which commonly led to infections necessitating antibiotic treatment and additional surgeries, innovative approaches were sought during the war. The dire situation prompted an Armenian Member of Parliament to seek assistance from Iceland, given their shared historical ties. Within a remarkable 72-hour timeframe, a plan was devised to ship supplies and deploy two doctors, Dr. H. Kjartansson from Iceland and Dr. S. Jeffery from the UK. Their mission was to provide training in the use of FSG (Fibrin Sealant Granules) for wound management. The primary objective was to utilize FSG to stabilize and improve the wound bed, facilitating the subsequent skin grafting process. This approach aimed to expedite healing time, enable earlier skin grafting, and achieve enhanced cosmetic outcomes throughout the healing process.
Fish Skin Graft Material and Method: A Revolutionary Approach to Burn Treatment
Fish skin grafts (FSG) derived from decellularized wild Atlantic cod skin, such as KerecisTM Omega3, have emerged as a promising biologic acellular matrix for burn treatment. These grafts maintain the integrity of the epidermis and dermis layers, preserving native Omega3 fatty acids due to gentle processing. With a shelf life of up to three years when stored dry at room temperature, FSG is easily rehydrated using saline.
FSG comes in sheets, averaging a thickness of 0.61mm ± 0.15mm, making it user-friendly and requiring minimal training for application. Its relative thickness provides a protective shield against environmental stimuli, reducing the risk of infection and acting as a dressing. Additionally, FSG contains intact Omega3 fatty acids, known for their antibacterial and anti-inflammatory properties. The versatility of FSG allows it to adapt to irregular surfaces and is available in pre-meshed sheets up to 300 cm2, with the capacity to stretch and cover up to 540 cm2. Utilizing larger sheets minimizes the need for joining and patching. Common techniques such as staples, negative pressure wound therapy (NPWT), or bolster dressings are employed to secure the graft in place. Postoperative dressing changes are typically performed every 3-5 days.
In adverse conditions, timely treatment for burn wounds may be challenging, and managing the wound until better care can be obtained becomes crucial. While rapid coverage and treatment are ideal to prevent long-term complications and preserve life and limb, FSG offers a viable alternative. The application of fish skin grafts has demonstrated favorable outcomes in burn treatment. Traditional approaches often involve autologous, allogeneic, or xenogeneic skin grafts. Fish skin grafts belong to the category of biologic dressings, serving as an effective cover for burn wounds. By reducing exudation, preventing infection, and alleviating pain, fish skin grafts expedite the healing process.
Although the use of fish skin grafts in burn treatment has gained recognition in coastal regions, it remains relatively unexplored in inland areas where human and porcine grafts are conventionally employed. However, recent studies have shown that fish skin, especially that of tilapia, contains abundant proteins and essential collagen, making it an excellent natural healing agent for burn wounds. Clinical trials conducted in Brazil have demonstrated the positive impact of applying sterilized and washed tilapia skin to burn injuries, promoting accelerated healing and preserving a moist, smooth wound bed without significant scarring.
Effects of fish skin grafts
During two treatment courses, several patients received fish skin treatment. Injuries included extensive full-thickness burns and blast injuries. Consecutively selected patients were admitted during the treatment. Most wounds were debrided once and had simple wet-to-dry dressings for 3-5 days before the initial application of FSG. Further debridement was performed when necessary. NPWT was applied after FSG, followed up in 7 days. At follow-up, patients were assessed for readiness for grafting. In all cases, FSG induced granulation of the wound bed days to weeks earlier, allowing earlier skin grafting surgeries to step down reconstruction and reduce the need for flap surgeries. There were no reports of infection in cases using FSG. Improvement in pain levels was not assessed. The doctors went to four other hospitals in the area to train surgeons in the use and application of FSG. Because FSG has a simple reconstruction and application procedure, making it easy to use, the training was easily adopted. Below we describe 4 cases using FSG to treat major blast injuries and burns.
Burn Treatment Case 1
Case 1 was a 19-year-old male with extensive full-thickness injuries from an explosion, including trunk burns. One of the injured had a large wound on the left heel with exposed bone. FSG was used in combination with NPWT. At the time of FSG application, most of the wounds were 8 days but had undergone initial debridement before the first application of FSG(Fish Skin Grafts).

This 19-year-old male had a left foot blown to the bone. No viable tissue was removed and a fish skin graft was applied, in combination with NPWT.
Burn Treatment Case 2
Case 2 was a 32-year-old soldier with a distal right tibial fracture. The patient presented with an open fracture and an external fixator was applied to stabilize the fracture. The fracture was associated with a large open wound (15 cm x 21 cm). The wound was debrided three times to ensure no viable tissue, fragments were removed and then FSG was applied. Follow-up was done every 3 days with the addition of new dressings. In total, three applications of FSG were done on the wound bed in preparation for thin skin grafting. The figure shows the initial wound presentation, application of FSG, and final intermediate thickness skin graft.

This 32-year-old male had a right lower tibial fracture with a large open wound. The fracture was stabilized, the wound was debrided, and the FSG was treated with a skin graft.
Burn Treatment Case 3
Case 3 was a 28-year-old male with full-body burns from a phosphorus explosion, with a total body surface area of about 75%. A total of 10 patients underwent debridement after hydro jet pressure washing. FSG was used as an alternative to skin grafting, which was successful.

This 28-year-old male with blast injuries had a TBSA burn rate of 75%. The wound was cleared before water jet pressure cleaning and fish skin grafting.
Burn Treatment Case 4
Case 4 Candido da Silva, a waitress at a restaurant in northeastern Brazil, adopted a new medical method after suffering severe burns to her arms, neck, and face in an explosion. The fish skin was implanted in her wounds, which were expected to heal quickly. According to reports, this was the first time scientists used fish skin to treat burn patients. Experts said that fish skin has anti-disease effects, can reduce infection rates, relieve pain, and act as a plaster. Before transplantation, professionals will do some treatment on the fish's skin. First, they will remove the scales, muscle tissue toxins, and any substances that may spread diseases from the fish skin, while removing the fishy smell. Then, the fish skin is stretched to 10 to 20 cm, cut into thin sheets, and stored in an icebox in São Paulo for up to 2 years. In this way, the fish skin will be similar to human skin, elastic, and easy to shape.

Da Silva, who is recovering after surgery, said: I feel like I'm in a science fiction movie. After the injury, I was in terrible pain and even felt desperate, but after the surgery, that helplessness disappeared. I like this treatment method and recommend that patients suffering like me try this fish skin.
Discussion
The austere environment experienced during wars and conflicts has posed considerable logistical obstacles to the treatment of injured soldiers. Treatment of wounds or burns, allogeneic transplants cooled for ultra-low storage is rare, meaning alternative approaches are needed. Treatment options on site need to be as shelf-stable as possible under a variety of environmental and climatic conditions. FSG has good features for use in such austere environments: the product is durable, lightweight, easy to transport, and requires few complicated tools or equipment beyond standard field medical equipment. In addition, with FSG, little training is required for rapid treatment of large numbers of patients, making it an ideal product.
The use of FSG allows granulation tissue to form earlier and better coverage of the underlying wound bed, with a low risk of infection. However, unlike dressings or other bridging measures, the use of FSG initiates the wound healing process rather than simply buying time. The presence of omega-3 fatty acids in fish skin may have an anti-inflammatory effect, enabling better revascularization of the wound bed and providing more favorable conditions for allogeneic transplants (although FSG itself is sufficient for healing some wounds). FSG has been shown to reduce implant time by half in pediatric patients. FSG can be used as long as sterile debridement tools, sterile saline, and room-temperature dry storage are available. Case reports show the practical results of exploiting these logistical advantages under such harsh conditions. However, this was not a controlled study, and given the nature of the patients, there were no documented pre-FSG assessments of the wound bed or extensive follow-up. Secondly, the combined use of NPWT and FSG (FSG is a standard and widely accepted procedure for treating surgical wounds with FSG) makes it difficult to truly evaluate the effectiveness of FSG in these patients. However, it should be noted that FSG is a CE-marked and FDA-approved product (several products available in the Kerecis Omega3 line), so its use in patients as described in this article is based on solid evidence rather than experimental theory.
Conclusion
This article describes the first successful deployments of FSGs in an austere environment. In this military context, FSG showed great portability and ease of knowledge transfer. More importantly, fish skin treatment showed faster granulation rates at grafting, thereby improving patient prognosis and no infection records. The concept of using fish skin in field hospitals and other military medical facilities should be further explored in a controlled environment, where more detailed analysis and assessment of secondary outcomes can be performed.
Some of the content and images in the text are copyrighted by:
1. Fouad Reda, MD, Hilmar Kjartansson, MD, FACEM, Steven L A Jeffery, MD, RAMC (V)
Military Medicine, usad028, https://doi.org/10.1093/milmed/usad028
© The Association of Military Surgeons of the United States 2023. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted reuse, distribution, and reproduction in any medium, provided the original work is properly cited.
2. COURTESY OF NATIONAL LIBRARY OF MEDICINE
3.Source:https://www.businessinsider.com/r-brazilian-doctors-use-fish-skin-to-treat-burn-victims-2017-5
#rhino #rhinorescue #burntreatment #Fishskingrafts